As Victorian residents are bracing themselves to see if positive coronavirus cases will rise even more, or start to descend, it's a different story on the other side of the world.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Victoria's increase still pales in comparison to the United States of America, which recorded 49,575 in a 24 hour period last week.
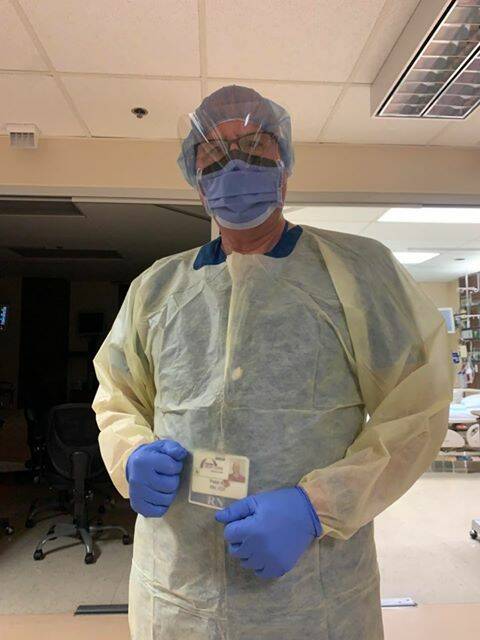
Almost 13,000km away from his home, former Wimmera resident Peter Alt is working tirelessly to treat the nation's most vulnerable.
He shared his story of hope, sacrifice and frustration with the Australian Community Media.
"I do 12 hour shifts in a six bed Intensive Care Unit," Peter said from his Marin County home, which is just 30 kilometres north of San Francisco.
READ MORE:
"Our team works with people who might have COVID-19 or people who have COVID-19.
"We use a lot of PPE (personal protective equipment); we're supposed to use different PPE for each patient, but we only get one N95 mask per shift.
"We are scratching for essential PPE and medication... we have to choose who gets Remdesivir (an antiviral drug).
"There's a squabble between state and federal authorities; I've heard the California authorities are flying PPE into remote locations to stop the feds from getting their hands on things.
"That's the same across the country."
The registered nurse said he and his colleagues were improvising to ensure their patients had the best chance of survival.
"The hospital would normally keep six months of of PPE and medication in supply, but it is gone in about 10 days," Peter said.
"I have to buy my N95 masks from hardware stores and chemists.
I see a lot more people getting COVID-19 before it goes away.
- Peter Alt
"We ran out of disposable gowns - the plastic gowns you see on TV all the time - so we're using one cloth gown per patient.
"I have a friend who wears a Tyvex suit to work everyday just to stay safe."
Mr Alt first began his nursing career at the Wimmera Base Hospital in 1985.
After stints in Melbourne and Perth, he ended up in California in 1990.
"I had sold all of my possessions to take up a new job in Saudi Arabia," Peter said.
"But then Saddam Hussein invaded Kuwait, and everything was off.
"With no possessions, I decided to move to LA to be a registry nurse.
"I worked a couple of months at each hospital, kind of like a locum in Australia.
"Eventually, I met my now-wife Inga, who is Norwegian, who is also a nurse.
"We now have three American children."

As of Thursday, California had more active cases (9231) than Victoria had recorded since the pandemic began (6289).
American public broadcaster National Public Radio has stated about 60,000 health care workers have contracted the coronavirus, something Mr Alt and his wife have gone to great lengths to avoid.
"My wife and I have a system for when we get home," he said.
"We get changed in the garage, put our shoes in chlorine, our clothing goes straight in the wash, and we have a shower.
"While we are doing everything we can at the hospital to make sure we are not infected, I don't want to risk my family at all.
READ MORE:
"Previously, if a staff member had coronavirus, they would be asked to stay at home; however, we are so understaffed, they can now work if they don't have any symptoms.
"I'm not in the right demographic (to die from COVID-19), but I still worry about passing it on to my children.
"I always ask myself 'Did I do the right thing today? Did I do everything right?'."
As an ICU nurse, Mr Alt is in the coalface of COVID-19, and he has seen more deaths than he would like to disclose.
While some deaths happen quicker than others, he said everyone who dies, does it alone.
OTHER NEWS:
"When someone is dying, there is no family, there is no one in the room with them," he said ruefully.
"We can do a video chat, but that is it.
"Some people don't believe in masks, but I can tell you everyone in ICU says they wish they wore masks.
"Unfortunately, I can't see this (the COVID-19 pandemic) ending any time soon.
MORE NEWS:
"I see a lot more people getting COVID-19 before it goes away."
Mr Alt estimated that the pandemic would end in September 2021 at the earliest.
He said people should seriously consider the permanent outcomes of implementing herd immunity.
"Let's say there's 15,000 people in Horsham," he hypothesized.
"To get herd immunity, we need at least 80 per cent of the population (12,000 people) to be exposed to COVID-19.
"With a mortality rate of one per cent, that means 120 people will die.
"Are we as a community prepared for that?"
He said a more straightforward approach could shorten statewide restrictions and lockdowns.
"My advice to the Wimmera: wash your hands, wear a mask, and socially distance," he said.
"It's the only thing that will stop the spread.
While you're with us, you can now receive updates straight to your inbox each Friday morning from the Stawell Times-News. To make sure you're up-to-date with all the news from across the Northern Grampians shire, sign up here.

